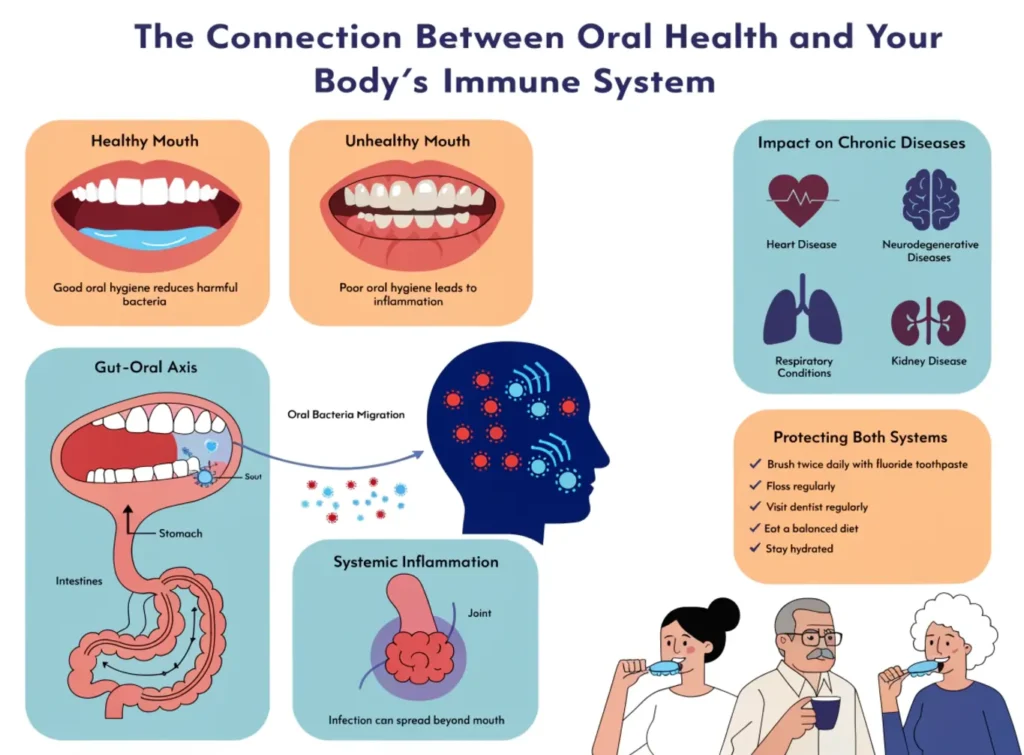
Most people think about oral health in terms of cavities, cosmetics, or the occasional toothache. That framing undersells what’s actually happening. The mouth is the body’s primary biological checkpoint – the first environment where pathogens either get neutralized or find a route into the rest of your system. What happens there doesn’t stay there.
How chronic gum disease taxes your defenses
Periodontitis is the best illustration of how a problem in your mouth is not just a problem in your mouth. When gum tissue breaks down, the epithelial lining – the physical wall between your oral environment and your bloodstream – develops gaps. Bacteria don’t need an invitation after that. They migrate through compromised gingival tissue directly into circulation, a process called bacteremia. Your immune system responds, but it has to keep responding, every day, because the source of the problem is still there.
This is what we mean by “perpetual alert.” T-cells and B-cells are being deployed continuously to manage an infection that never resolves. That draws resources away from everything else – seasonal viruses, early-stage pathogens, normal immune surveillance. People with untreated periodontal disease don’t just have a gum problem. They have an immune system that’s been slowly worn down.
Individuals with periodontal disease have significantly higher serum levels of C-reactive protein compared to those with healthy gums, indicating oral bacteria directly contribute to systemic inflammation. CRP is a reliable marker for this kind of low-grade, chronic inflammatory load – and chronically elevated CRP is the same profile associated with cardiovascular disease and poorly managed diabetes. The connections aren’t coincidental.
When a dental emergency becomes a systemic threat
Abscesses are on the opposite end of the spectrum. Although it’s a localized infection, that doesn’t mean it’s contained. The bacteria causing the infection can travel along tissue planes to the jaw, neck, or chest. They may also enter the bloodstream and create a systemic infection. At that point, this is no longer a tooth issue, it’s a sepsis risk as the immune system fights bacteria that’s reached systemic circulation.
That’s why time is of the essence. If someone has a swollen jaw, severe throbbing pain, or a visible abscess, waiting it out is a real risk. Searching for an emergency dentist near me at that point is not an overreaction – it’s the step that keeps a localized infection from causing an acute immune response that is hard to manage at home or with antibiotics.
The immune system’s pro-inflammatory proteins (cytokines) released in response to an acute dental infection don’t respond to the size of an abscess – they just know the body is in danger. Too many of them being produced too fast, and it’s not just your tooth that’s going to be at risk – those proteins will start damaging healthy tissue as well.
Saliva does more than most people realize
Saliva is not just a liquid in your mouth. It actually harbors salivary IgA, a defense antibody that grabs microbial invaders before they can enter your gut or your lungs. Saliva also contains enzymes that bust open bacterial cell walls and interfere with their ability to form communities or “biofilms”. If your flow of saliva is good and your mouth’s population of microbes is within a healthy range, this is a robust front-line defense against invaders.
Speaking of the mouth’s population of microbes, it’s a very varied biome in its own right. But it’s not just a numbers game: if the microbial biome is nice and stable, the likes of _Porphyromonas gingivalis_ can’t get the upper hand. When the biome gets disturbed – by the overzealous use of antibiotics, by not having great oral hygiene, or through low-level chronic inflammation – the ecosystem gets out of balance and your immune system has to pick up the slack.
Practical management that actually works
Biofilm – the bacterial film that accumulates on teeth and below the gumline – is the root of most of this. Brushing and flossing aren’t just hygiene habits. They’re the primary mechanism for disrupting biofilm before it mineralizes into calculus, which the immune system genuinely cannot remove on its own. Once calculus forms, professional cleaning is the only way to clear it.
Two things make a real difference here. Consistent daily biofilm removal keeps the bacterial load manageable and prevents the gingival tissue from reaching the breakdown point where bacteria can enter circulation. Professional cleanings go further – they remove calcified deposits below the gumline that brushing physically can’t reach, and they give a clinician the chance to catch early-stage periodontitis before it becomes chronic.
The other variable is response time when something goes wrong. Acute dental infections don’t benefit from patience.
Dental care as immune maintenance
A dentist does not just manage teeth. Biologically, regular dental care is one of the most direct ways to help prevent systemic inflammation. This is probably not the view most people think of when going to the dentist, but it is in fact true. If the mouth is the gatekeeper, then maintaining it means maintaining everything else functioning.